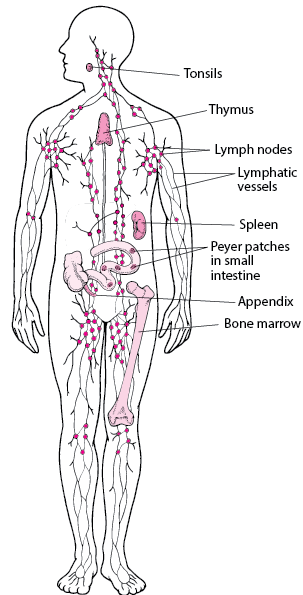
Staying on topic with complications after breast cancer surgery. The two I’ll discuss today are common and can be disruptive to daily life. You’ve probably heard of frozen shoulder (adhesive capsulitis), but you may not have heard about breast capsulitis after breast reconstruction. Let’s dive in a little deeper.

What is capsulitis?
Capsulitis is inflammation of a joint capsule or the capsule around a breast implant that can lead to scar tissue adhesions and stiffening or immobilization of the joint or breast capsule. Uncomfortable – yes. Functionally limiting? Also, yes.
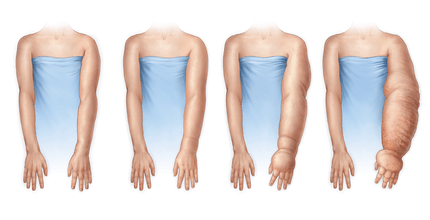
Frozen shoulder
While frozen shoulder (adhesive capsulitis) can occur after any shoulder injury, it can occasionally occur without any injury, and is more common in females and in people with diabetes mellitus or hypothyroidism. Frozen shoulder typically presents as a significant loss of motion in the shoulder with or without pain. To read a bit more about frozen shoulder, click here.
After breast cancer surgery, frozen shoulder is also common. For women aged 50-59, women who had mastectomy, or women who had breast reconstruction, the risk of developing frozen shoulder on the affected side is approximately 10%.1
Functionally, frozen shoulder leads to difficulty getting dressed, showering, combing your hair, lifting and carrying objects, driving, sleeping, and a whole lot of things we do on a daily basis.
Physical therapists treat frozen shoulder using manual therapy like joint mobilizations, teaching passive stretches and gradually strengthening around the joint as motion improves, and educating patients on healing timeline and ways to modify daily activities to improve use of the arm and reduce pain.
Rehab for frozen shoulder can sometimes take close to a year before a person feels “back to normal.” If caught early enough (i.e. during the “freezing phase” when motion loss begins to occur), a steroid injection can help to minimize the symptoms and restrictions. See your doctor right away if you notice a major loss in joint motion after breast cancer surgery.
Post-reconstruction capsulitis
Post-reconstruction capsulitis or capsular contracture can occur when fibrotic changes occur in the tissue capsule that forms around new breast impants. The breast around the new implant hardens, can become painful, and the breast shape can become distorted. To read a bit more about capsular contracture, click here.
Risk for developing capsular contracture is higher after radiation therapy or following infection, hematoma, or seroma that develops around a new implant. It is not clear whether smooth versus textured implants play a role in development of capsulitis.
Typically, if capsulitis occurs and is painful, distorts the breast shape or an underlying infection is present, revision surgery is needed. In Australia, approximately 39% of revision surgeries each year are due to capsular contracture.2 With early stage contracture, a physical therapist can use manual therapy to try to restore motion and prevent further fibrosis of the breast. A PT will also be sure to address shoulder, neck, and chest wall motion which could be compromised with post-implant capsulitis.
For both frozen shoulder and post-reconstruction capsulitis, getting into see a physical therapist early is important to prevent loss of motion and to reduce pain. Ideally, PT’s would love to see breast cancer patients within 4-6 weeks after breast surgery or reconstruction. Developing a relationship with a physical therapist during and after breast cancer can be a great asset to your health and wellness beyond cancer. Ask your surgeon for a referral or find a PT in your area here.
Aloha ❤