It’s no secret that I am freakishly in-tune with my body and that I also value knowing exactly what’s happening behind the scenes of my symptoms. Even before I was diagnosed with breast cancer, I knew something was off with my body, and I’d started to research root causes and naturopathic/functional medicine approaches to help me with some things I’d been experiencing. Then, cancer came into my life and between the 85 million appointments (not exaggerating…), I decided to hold off on seeing yet another practitioner.
Now that I’m approaching the end of active cancer treatment, I decided it’s time to get some additional support and testing done. A few things I was concerned about include the health of my digestive system, support for my thyroid, and restoring equilibrium for my female hormones. I chose to see a naturopath (ND) based on recommendations from friends and based on her experience level and social media content (never underestimate the power of social media!). Here’s a few things I’ve learned after my initial consultation and lab work:
Get that Good Gut Health
Chemo is designed to destroy cancer cells which are typically rapidly dividing and multiplying in our bodies. Well – guess what else rapidly divides and multiplies? Healthy cells in our digestive tracts! Side effects from chemotherapy tend to hit the GI tract hard and can include mouth sores, nausea/vomiting, heartburn, and diarrhea or constipation. Seeing as I had several of these symptoms during my 16 rounds of chemo, I knew my gut was going to need support and healing.
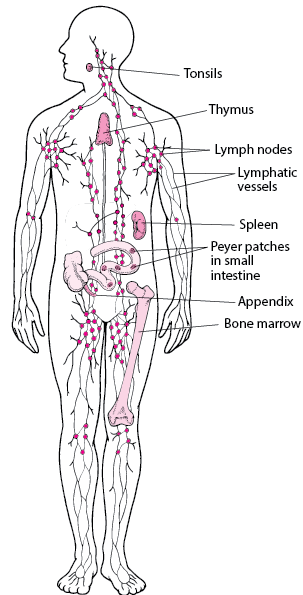
First of all, the GI tract is full of trillions of happy, healthy bacteria typically referred to as the gut microbiome. These bacteria help us to digest food and maintain a strong immune system. It’s all a bit complex honestly, but a lack in diversity of these bacteria can lead to a whole host of health issues, including mental health concerns.
My ND recommended a few important things to get me started: a good probiotic to promote microbiome diversity and a drink called GI Revive which supports the intestinal lining and promotes regularity. It’s also crucial to eat a diverse, supportive diet that includes plenty of fiber, vegetables and whole grains, and fermented foods.
*Side note – if I’d known GI Revive existed, I would have started it during chemotherapy. However at that time, I did use L-glutamine supplements which helped me prevent issues in my mouth and lower GI tract.
Altogether, I feel like things are coming back around to normal after chemotherapy with this added support. I imagine that the more my gut heals, the more I’ll see my immune system improve and I’ll be able to maintain low levels of inflammation in my body.
Clarity on Chemopause
I started chemo on June 9, 2020, and that was also the first day I received a Zoladex injection. Zoladex is a hormonal therapy designed to stop the ovaries from creating follicles which release estrogen. The ovaries have a high rate of cell turnover like the GI tract, so chemotherapy can lead to infertility if not protected by hormonal therapy. Modern medicine is truly incredible, and I’m grateful that as a 30-year-old woman going through chemo, I had the option to try to save my fertility in this way.
Joke’s on me though, because after 6 months of this hormonal therapy, I am officially in chemopause (a medically-induced menopause), and I have all the symptoms to show for it. I specifically asked my ND for post-chemo baseline labs for my estrogen, progesterone, and testosterone levels. No surprise here, but my labs confirm I’m in a menopausal state and that explains the hot flashes, joint pain, dyspareunia (learn more here), and amenorrhea…
Now, true menopause means a woman has had no menstrual cycle for >12 months. Being only two months out from my last Zoladex injection, I’d say there’s still hope for my ovaries to bounce back. Most women who’ve been on this type of treatment have seen their menstrual cycles return after 5-6 months on average. In the meantime, I need to be supportive of my body! I attempt to exercise 3-5 times per week (walking, resistance training, and stretching) to relieve joint pain and both my ND and OB/GYN have recommended vaginal moisturizers to prevent vaginal atrophy until my estrogen levels improve. (If this is TMI for my family & friends reading this – sorry, but it’s just #RealTalk!)
I’ll continue to monitor my labs every few months to be sure things are trending in the right direction. Chemopause isn’t necessarily permanent, so here’s hoping my body can pull through!
The Thyroid Needs to Thrive
About seven years ago, while I was deep in PT school, I began having unnatural fatigue. I ended up being diagnosed with an underactive thyroid gland (hypothyroidism). The thyroid gland produces hormones which help regulate our metabolism, and if the thyroid isn’t functioning optimally, you can have symptoms like fatigue, dry skin, hair loss, weight gain, constipation, or feeling like you’re always cold. Every body system relies on the thyroid so it’s a priority to take care of it!
Trying to find the root cause of my thyroid dysfunction has always been something I was curious about before my cancer diagnosis, and after treatment I wanted to know if there was: a) any additional support needed for my thyroid after chemo, and b) if there was an underlying cause for my hypothyroidism. After running a full thyroid panel, my ND diagnosed me with Hashimoto’s thyroiditis, an autoimmune condition in which my own immune system is attacking my thyroid. She educated me that Hashimoto’s is actually the most common cause of hypothyroidism and affects about 5 in 100 people.1 It seems that Hashimoto’s is a combination of genetic factors and environmental factors such as food sensitivities or heavy metals toxicity.
My next step is to try to determine what may have triggered this autoimmune condition. The more I know about my condition, the better I can treat it or avoid any sensitivities that may make my condition worse. It might seem like I am seeking out more health problems, but my intent is really to understand my own body and how I can best support it to remain healthy and cancer-free. I will likely always have to be on thyroid medication, but I’d like to try to prevent the condition from progressing as much as I can (I plan on living a long life, you know?!).
Sometimes You Just Have to Supplement
In all honesty, I’ve never been a fan of supplements because I just can’t remember to take them every day! I now understand, however, that there are certain vitamins and minerals that I’m unable to get enough of through a vegan/vegetarian diet (like vitamin B12 which is only found in animal products), and also, based on my recent lab work, we found that some others (like my vitamin D and zinc levels) were significantly depleted for me during chemotherapy.
There are certain supplements I need to be cautious taking during radiation therapy as high levels of antioxidants (like those in vitamins A, C, and E) can interfere with the treatment itself. For now, I am supplementing with:
- B vitamin complex to improve my energy levels and cognitive functioning
- Vitamin D3 which promotes bone health and has been shown to reduce the risk of cancer metastasis
- Omega-3 which helps to reduce inflammation and supports brain and heart function
- Zinc which supports the immune system
- A probiotic and the GI drink I mentioned earlier for gut health
It sounds like a lot, but I’m currently finding it very worthwhile. Some of the brain fog that started during chemo has lifted since I started supplementing more regularly, my GI system is more settled, and my hair is growing back much faster than I anticipated! Maybe eventually I won’t need so much supplementation, but I feel now is the time to be very supportive of my body and it’s healing.
The Cost of Collaborative Care is: Priceless.
I know what you’re all thinking – this all sounds expensive! And it is to some extent. Supplements can be pricey & aren’t covered by insurance like most pharmaceuticals. When providers don’t contract with insurance companies, the costs can add up. I don’t need to explain myself, but I just want to let you all in on my thought process at this point.
Seeing an ND and using supplements and acupuncture to support my healing have brought me immense benefits and peace of mind both before and after my cancer diagnosis. I personally feel that seeing a fee-for-service provider is excellent because they are not held to unreasonable standards that insurance companies often dictate. These providers can spend more 1:1 time with their patients, can recommend tests and treatments that can be run through insurance companies, and can provide a more holistic approach to your care. I personally feel it worth every penny to have this kind of care.
If you don’t have your health, you have nothing. This year my body has been through the ringer and besides feeling physically unwell, I saw my mental health and my relationships challenged. I was hardly able to concentrate on anything besides getting through treatment and managing my symptoms. My husband became a “caregiver” and most of our life revolved around what I could and couldn’t do with friends during a pandemic when you’re immunocompromised. I haven’t been able to treat patients for almost a year and so my sense of purpose got a little muddy at times.
Now is the time for me to heal from all of that. I am beyond grateful for good health insurance that got me through treatment without any debt, family and friends who contributed to my GoFundMe so I can seek out alternative care options as I continue to heal, and for my super-supportive coworkers who’ve donated time off and kept me in the loop at work so I don’t feel like a complete outsider. These things may seem small, but they can mean the world to someone living with a complex illness.
Again, my purpose here is to share my journey in case someone else going through this can benefit from what I’ve learned. Much of this info is very personal, and I choose to be open about this. I’ve said this before, but just because someone is considered “cancer-free” doesn’t mean they’re not still experiencing some of the long-term effects of treatment. We use fire to fight fires in cancer care and there are often side effects of side effects!
Please be kind! If you know someone in treatment (or if you know someone who may just need a little extra help), reach out today and see how you can support them – we’ve all got to have each other’s backs.
Aloha ❤
*This post is not intended to provide medical advice or recommendations. I am simply stating what has worked or been recommended to me on my personal journey. For more information, read my full disclaimer here.